BITS Hyderabad researchers target obstinate bacterial refuge in body called ‘biofilm’
Infections that return even after a full course of antibiotics remain one of health care’s toughest challenges. A new laboratory study from BITS Pilani’s Hyderabad campus explores a strategy that may help existing antibiotics work better against bacteria hidden inside protective biofilms.
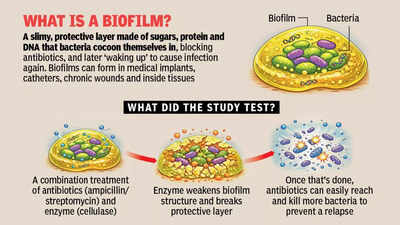
Findings of the study, titled ‘Breaching the biofilm fortress’, were published in the Chemical Engineering Journal in March.Biofilms are structured communities of bacteria encased in a self-produced protective layer made of sugars, proteins and DNA. This slimy matrix attaches to surfaces such as catheters, implants and chronic wounds, acting like a shield that blocks antibiotic entry. And even when antibiotics kill most bacteria, some cells survive in a dormant state and later ‘wake up’, causing infections to return.
While many studies focus on reducing biofilm mass, this research shifts attention to preventing that post-treatment comeback.“By targeting the structure of the biofilm, the approach aims to limit the survival of dormant cells that can cause relapse,” says study author Ramakrishnan Ganesan from the chemistry department of BITS Pilani’s Hyderabad campus, adding that the findings underline the importance of attacking the protective matrix itself.
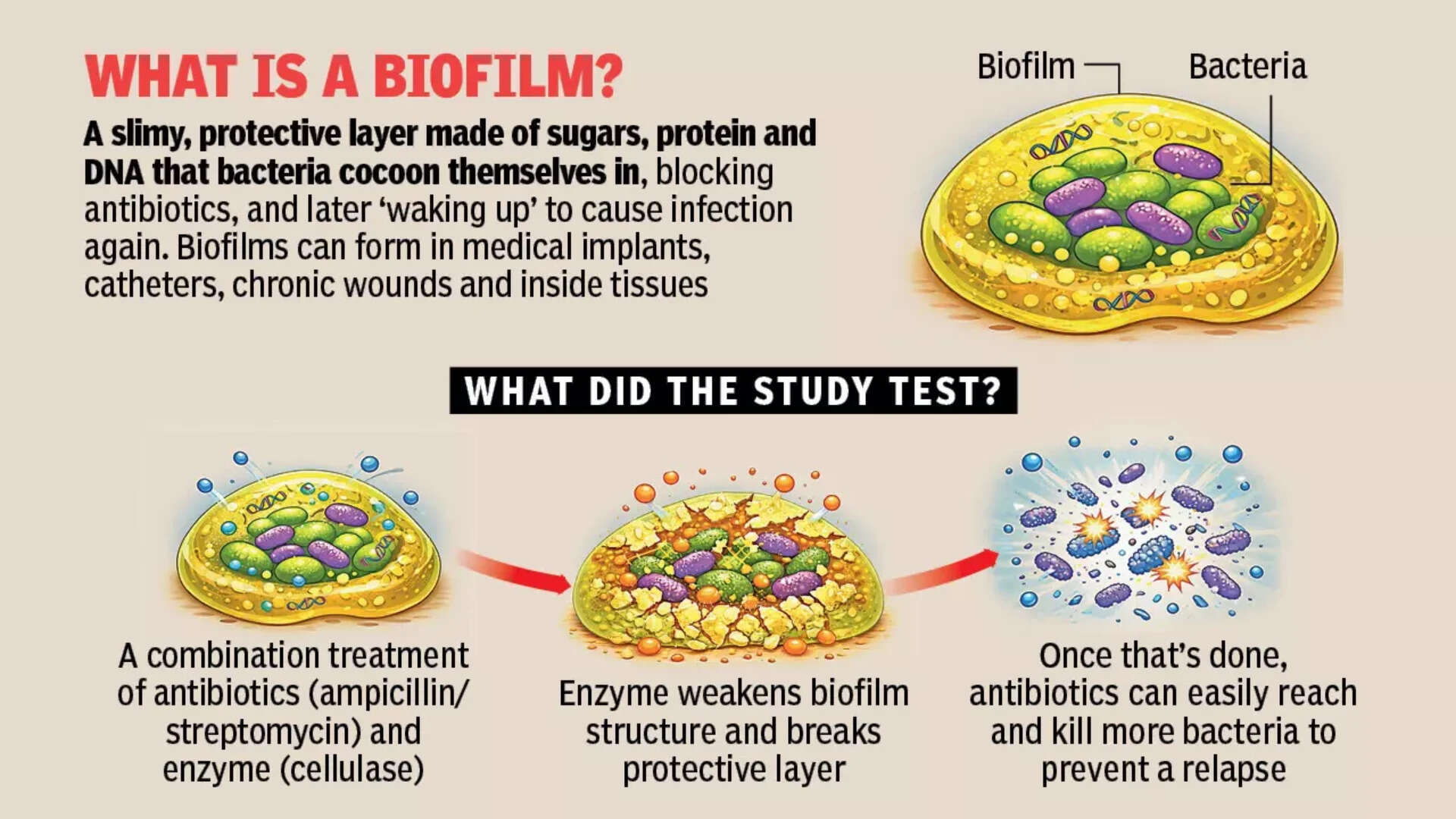
To test the approach, the team isolated a naturally occurring, biofilm-forming E coli strain from near Patancheru Lake on the outskirts of Hyderabad, an area exposed to diverse industrial and pharmaceutical effluents. The strain was found to be closely related to sequence type 10 (ST10), a lineage known for both harmless and disease-causing variants. By using an environmentally derived strain rather than a stable lab strain, the researchers aimed to better reflect real-world bacterial behaviour.The study evaluated two widely used antibiotics — ampicillin and streptomycin — both alone and in combination with cellulase, an enzyme that breaks down polysaccharides in a biofilm matrix. The idea was simple: weaken the barrier first, then allow antibiotics to penetrate more effectively. Across repeated treatment cycles, the combination therapy performed significantly better than antibiotics alone. Among the treatments tested, the streptomycin-cellulase pairing delivered the strongest results, achieving near-complete removal of viable biofilm cells under laboratory conditions.Imaging techniques confirmed extensive breakdown of the protective matrix, allowing improved drug penetration. Safety tests conducted on mammalian cell lines showed over 90% cell viability, suggesting good biocompatibility at the experimental stage. “Suppressing biofilm resuscitation — rather than reducing biomass alone — is key to overcoming antibiotic treatment failure,” says the study.Jayati Ray Dutta, a professor at the biological sciences department and another researcher in the study, points out, “The study suggests that breaking down the biofilm barrier, rather than relying only on higher antibiotic doses, could provide an additional strategy to manage persistent infections in healthcare settings.” Further studies are needed before the approach can move towards clinical application.

